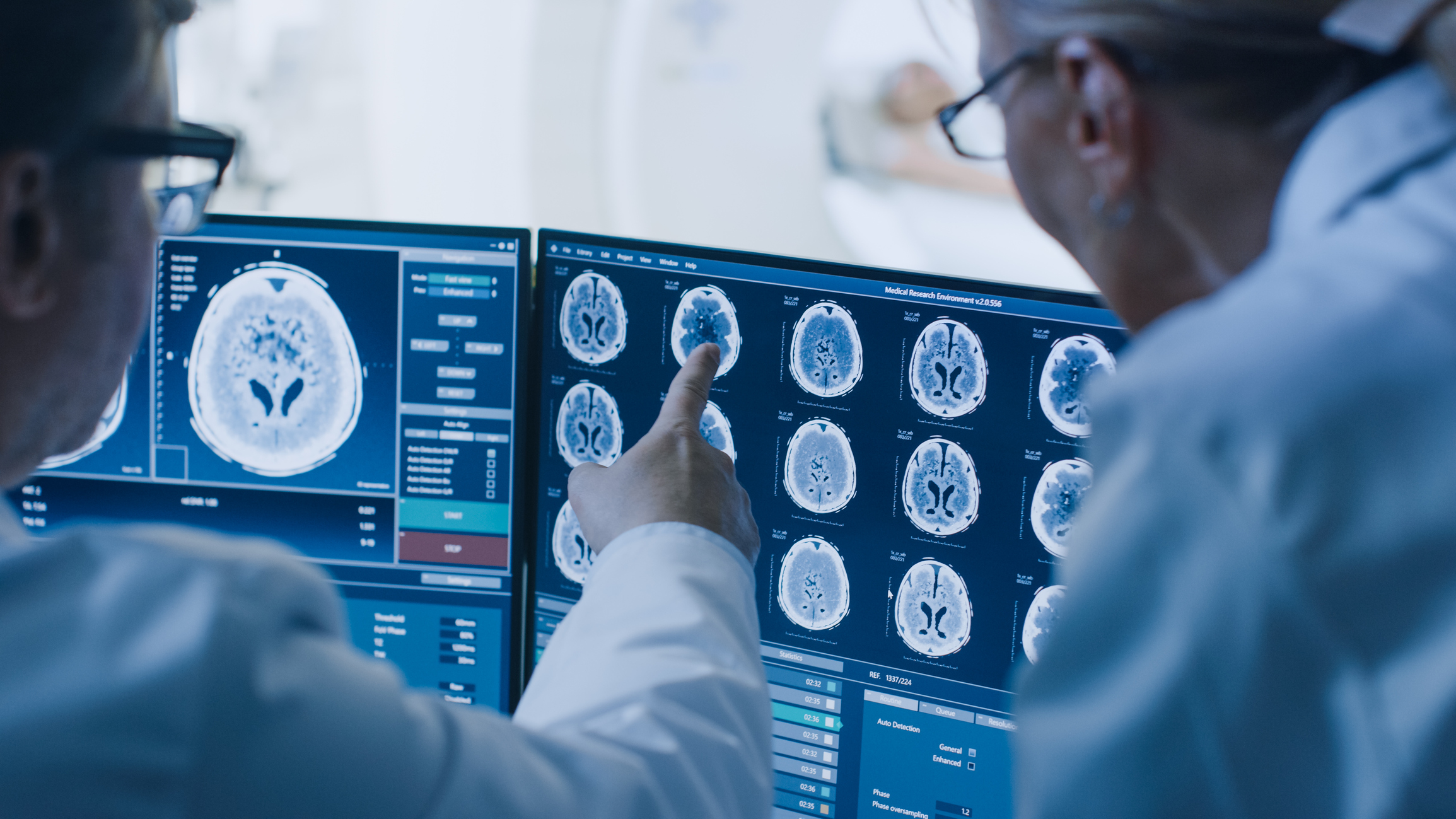
TeleNeurology is an emerging field that utilizes telecommunications to diagnose and treat neurologic disorders. It links neurology specialists, who are often located in different locations, with patients who can be thousands of miles away. Bedside staff and patients are able to interact with the specialist through videoconferencing or voice-over-internet protocol (VOIP) technology. Previously, the main purpose of telemedicine is to help bridge the gap between clinicians and patients living in rural areas, where access to medical care may not be readily available or affordable.
But the pandemic ushered in a new era of telehealth — as it was used as a measure to ensure both patient and staff safety, preserve valuable PPE, as well as support healthcare systems with staff coverage and burnout. As of 2020, about 75% of U.S. hospitals were using telehealth and telemedicine systems—a 42 percent increase from 2019 usage, according to Definitive Healthcare.
Aging Population:
When we examine the facts, we can observe that human life expectancy has increased dramatically in recent decades. Our average lifespan was 30 years in the previous century, but thanks to technological advancements, we can live up to 83 years on average today. According to the United Nations, there will be around 2.1 billion individuals over the age of 60 by 2050 — that’s a quarter of the world’s population. Anyone above the age of 60, on the other hand, will have various morbidities, the most prevalent of which are cardiovascular illnesses, followed by malignant neoplasms, chronic respiratory stress, and so on.
We see a significant curve of varying illness loads at various age ranges in neurology (1). Encephalitis and meningitis are common in children and infants, but as we get older, migraine, multiple sclerosis, and headaches become more common. For people of older ages, stroke and Alzheimer’s disease take control. People are often forced to live with these disabilities, resulting in a decrease of quality of life. We urgently require additional neurologists to care for our aging population.
Lack of Neurologists:
Unfortunately, there will be a severe shortage of neurologists in comparison to what we require. In fact, by 2025, there will be a 19% deficiency. That’s only four years away, and it’s only going to get worse. The major difficulty is that, as seen in the map below, rural areas (colored red) are the ones that require the most attention, but will be the most underserved (2). Except for a tiny corridor in the northeastern region, there will be a shortage of neurologists everywhere. As a result, there will be a severe demand-supply imbalance. So, how are we going to give neurological treatment in those areas? There’s only one solution and that is TeleNeurology. With telehealth, we can virtually care for these patients and help them appropriately.
Related: Telemedicine Neurology: A Stroke of Genius
Virtual Care is Healthcare:
The scarcity of neurologists emphasizes the need for virtual care, and we must increase the virtual presence of neurologists. This will allow them to quickly shift from one hospital to another, saving them time in terms of transportation, parking, and so on. The notion that in person care is vastly superior to virtual care is quite outdated . We must recognize that both are highly valuable, and it is therefore preferable to employ virtual care for first examinations. Physicians can use tele-visits to advise their afflicted patients on whether or not an in-person visit is worth their time. Due to recent technological advancements, we can now transport labs, x-rays, and even portable MRIs to distinct rural communities. We should remove these barriers, especially in relation to travel, and make virtual treatment universal.
Roadmap for TeleNeurology Success:
To achieve teleneurology success, telehealth companies need to understand that the practice can be divided into these two areas:
1. Acute Care Setting
2. Chronic Care Setting
In acute care settings, we need to concentrate on the systems of care, because we’re taking care of stroke patients, neuro ICU patients, or inpatient neurology concepts. In that setting, we need to understand how the systems of care will be evaluated; in addition to the physician, we also need to concentrate on the three Cs — Collaboration, Communication, and Crew (teamwork).
Now, when their stroke is initiated, it could be in a primary stroke center, which needs to be transferred to a comprehensive stroke center for thrombectomy. So what we need to concentrate on is a secure messaging platform or remote teleradiology, viewability of EMR through different platforms so that we can provide timely care. These require protocols and systems of care thinking — where teleneurology is part of the core team, and not just an auxiliary part of the team.
In chronic care settings, a multi-party view is extremely important. In situations where a patient has had a stroke, cognitive decline, or Alzheimer’s disease, physicians might need more information that only a patient’s family members would be able to provide, and we should be able to get in touch with them directly through the multi-party system. We also need to make sure it’s easy for elderly people to get on board and get the help they need with just a single click. There should be either SMS, text, or even an email reminder system. And more importantly, there should be an educational platform due to which not just the patient, but even his/her family members are prepared for it.
For teleneurology to be a success, the systems must be robust and reliable, with a rapid response time. Camera systems and other acute care systems need to be excellent in quality, especially in the acute care setting due to the need for pupillary, tremors, and gait exams. The UI involved should benefit both the patient and physicians. The system needs to be fast and be compatible with all operating systems.
VeeOne Health
We’ve included all of these features in VeeOne Health as well. We provide a one-stop-shop for healthcare systems seeking a healthcare platform for the entire continuum of care — inpatient, outpatient, remote patient monitoring, as well as solutions for ICU, stroke treatment, and other care needs. In addition to a reliable, secure, and truly integrated platform, we also provide operations support, as well as physician services — including teleneurology, telepsychiatry, telehospitalist, tele-ICU, and even tele-neurosurgeons, among other specialties.
We recognize the need for virtual care in the future and we want to be at the forefront. People will be able to get the care they need no matter where they are, and physicians will be able to help people in various hospitals without needing to travel.
To get more information about VeeOne Health’s teleneurology solutions, or our other products and services, please feel free to contact us to set a up a free demo or consultation: https://veeonehealth.com/contact/
Related: A Guide to the Functions, Use, and Value of the Telemedicine Cart
Dr. Junaid Kalia is Vice President of Clinical Strategy at VeeOne Health, specializing in Tele-Neurocritical Care, Stroke & Epilepsy.